Residents of Idaho seeking a non-hormonal contraceptive option might find the CAYA diaphragm to be an excellent choice. This guide outlines the steps and state-specific requirements to help you obtain the CAYA diaphragm in Idaho.
To get the CAYA diaphragm in Idaho, start by scheduling an appointment with a licensed healthcare provider. Idaho law requires a prescription for the CAYA diaphragm, so you'll need a healthcare professional to assess your suitability for this contraceptive method. During the consultation, your provider will review your health history and explain how the CAYA diaphragm works.
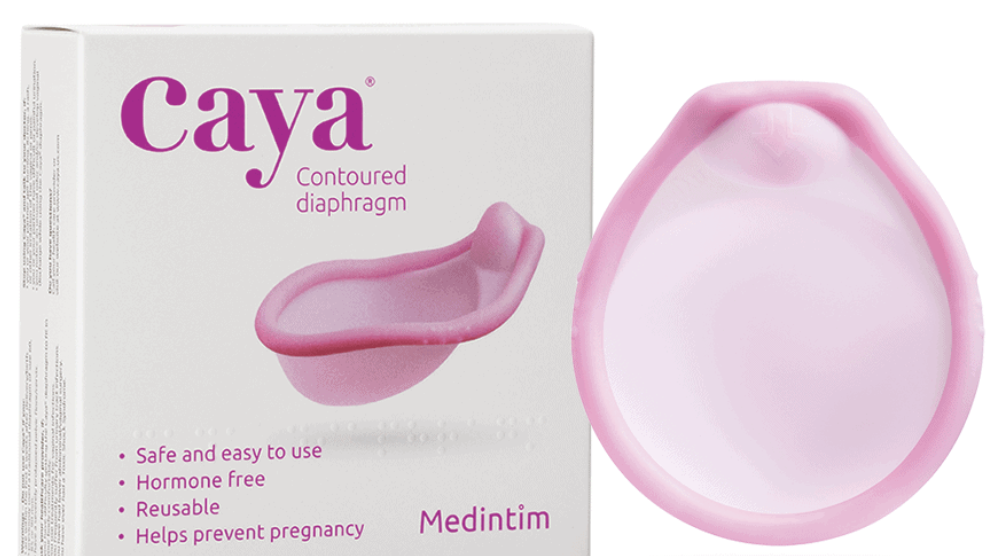
In Idaho, obtaining the CAYA diaphragm requires a prescription. Once your healthcare provider determines that the CAYA diaphragm is suitable for your contraceptive needs, they will issue a prescription. If your usual provider is unfamiliar with the CAYA diaphragm, you may seek out a clinic or provider specializing in non-hormonal contraception within the state.
With your prescription, the next step is finding a pharmacy in Idaho that carries the CAYA diaphragm. Not all pharmacies stock it, so calling ahead or searching online for availability is recommended. You can also opt to order the CAYA diaphragm from an online pharmacy that ships to Idaho.
Idaho health insurance plans, including those under the Affordable Care Act, often cover contraceptive devices like the CAYA diaphragm. Before purchasing, confirm with your insurance provider if the device is covered. If you're uninsured, Idaho's Medicaid program or other state-assisted health plans may cover the CAYA diaphragm.
Using the CAYA diaphragm correctly is essential for its effectiveness. Your Idaho healthcare provider should offer you detailed instructions on how to use the CAYA diaphragm, and online resources are available to help ensure proper usage for maximum contraceptive benefits.
My Virtual Physician offers telehealth appointments for patients interested in the CAYA diaphragm. Schedule your appointment with us today! BOOK HERE
If you're in Florida and considering home insemination with fresh frozen sperm, this guide provides an overview of the steps and state-specific requirements you need to follow. Home insemination is a growing trend for individuals and couples hoping to conceive, and using fresh frozen sperm can improve your chances of success. Here’s how you can access fresh frozen sperm for home insemination in Florida.
In Florida, home insemination is legal, but the sperm used must come from a licensed sperm bank to ensure it has been properly screened. Florida mandates that sperm donors undergo thorough testing for infectious diseases, such as HIV, hepatitis, and sexually transmitted infections (STIs), to ensure the safety of both the recipient and any future children.
To get fresh frozen sperm for home insemination in Florida, you'll need to work with a licensed sperm bank. Make sure the sperm bank complies with state and federal regulations regarding donor screening and sperm processing. Many banks provide comprehensive donor profiles that include details such as genetic history, physical attributes, and even personal interests.
Since not all sperm banks deliver to Florida, verify that the bank you choose can ship fresh frozen sperm to your location. The sperm bank will ship the sperm in a specialized container designed to maintain the required frozen conditions during transport.
In Florida, most sperm banks require a prescription from a licensed physician before releasing fresh frozen sperm for home insemination. Schedule an appointment with a healthcare provider in Florida to discuss your insemination plans. Your doctor will ensure that home insemination is appropriate for your situation and provide the necessary prescription.
After selecting a sperm donor and obtaining your prescription, place your order with the sperm bank. When ordering fresh frozen sperm, be sure to coordinate the delivery with your ovulation cycle for optimal results.
The sperm bank will ship the fresh frozen sperm in a container designed to keep it frozen until it reaches you. It’s essential to follow the sperm bank’s instructions for thawing and handling the sperm correctly to ensure the best chances of conception.
Once your fresh frozen sperm arrives, you can proceed with the home insemination process. Follow the instructions provided, which may include using a sterile syringe or other equipment sent by the sperm bank. For advice on timing and technique, consider consulting your healthcare provider to improve your chances of conception.
In Florida, anonymous sperm donors generally have no legal rights or responsibilities toward children conceived through sperm donation, as long as the sperm is obtained from a licensed sperm bank. However, you should consult with a legal expert familiar with Florida reproductive laws to ensure that you fully understand the legal aspects of home insemination.
Home insemination with fresh frozen sperm can be a successful family-building option for individuals and couples in Florida. By following the state's regulations and choosing a licensed sperm bank, you can safely proceed with the insemination process. Always consult a healthcare provider to determine whether home insemination is right for you and to receive guidance along the way.
My Virtual Physician offers telehealth appointments for patients interested in home insemination. Schedule your appointment with us today! BOOK HERE
In today's fast-paced world, the importance of accessible and high-quality health care cannot be overstated. At My Virtual Physician, we are committed to revolutionizing the way patients receive medical care, making it more convenient, efficient, and effective. As we continue to grow and innovate, we are excited to announce our RegCF (Regulation Crowdfunding) campaign and we would love for you to be a part of this unique transformative journey.
Dr. David Howard, the visionary, founder, and sole stakeholder, has remarkably bootstrapped My Virtual Physician while balancing demanding hours in a hospital's labor and delivery department. Over the past four years, Dr. Howard's dedication and strategic growth efforts have propelled the company to achieve sustainable and substantial success.
Dr. David Howard was born in Jamaica and immigrated to the U.S. at eighteen years old. Dr. Howard received his Bachelor of Arts in Psychology from the Johns Hopkins University and then pursued his Md and Ph.D. in Epidemiology through the Medical Scientist Training Program at the Johns Hopkins School of Medicine.
My Virtual Physician is a national, multi-specialty telehealth company that connects patients with board-certified and licensed physicians through its secure, user-friendly virtual platforms. Our services span various specialties, including primary care, pediatrics, women's health (Gynecology), and more, ensuring comprehensive healthcare solutions for individuals and families across the US.
The healthcare landscape is rapidly evolving, and the demand for telehealth services has never been greater. By launching a RegCF campaign, we aim to:
1. Expand Our Reach: With your support, we can extend our services to underserved communities, providing vital healthcare access to those who need it most.
2. Enhance Technology: Investing in cutting-edge technology will enable us to offer even more innovative solutions and improve patient experiences and outcomes.
3. Grow Our Team: By attracting top talent in the medical and technological fields, we can continue to deliver exceptional care and drive forward our mission of making healthcare more accessible.
Participating in our RegCF campaign means contributing to a future where quality healthcare is
within everyone's reach.
This year our goals are to:
1. Develop New Services: Expand our national reach by adding even more specialty services to offer our patients.
2. Improve Patient Experience: Enhancing our virtual platform and website to ensure seamless and efficient consultations.
3. Foster Community Health: Create initiatives and partnerships that promote health and well-being in underserved communities.
Getting involved in our RegCF campaign is straightforward and accessible. By visiting our campaign page https://netcapital.com/companies/myvirtualphysician, you can learn more about our mission, vision, and growth plan. Your support, whether large or small, will make a significant difference in helping us achieve our goals.
Join Us in Shaping the Future of Healthcare
Thank you In Advance For Your Support,
David L. Howard, M.D., PH.D, CEO, OBGYN
Pelvic pain is a common symptom that can have various underlying causes, ranging from menstrual cramps to more serious conditions like endometriosis or pelvic inflammatory disease (PID). Consulting with an online Ob/Gyn doctor can offer valuable support and guidance in managing pelvic pain effectively. Here's how:
Scenario 1: Emily sat at her desk, her face creased with worry as she typed into her laptop, seeking answers to the persistent pelvic pain that had plagued her for weeks.
Emily: Typing furiously "Pelvic pain causes..."
After scrolling through various search results, Emily stumbled upon an online Ob/Gyn consultation service. With a glimmer of hope, she clicked the link and scheduled an appointment for a virtual consultation.
The next day, Emily settled into her cozy armchair, laptop open, awaiting her online appointment. A cheerful chime signaled the start of the consultation.
Dr. Hernandez: "Good afternoon, Emily. I'm Dr. Hernandez. How can I assist you today?"
Emily: Rubbing her temples "Hi, Doctor. I've been having this persistent pelvic pain for a while now, and it's really starting to worry me."
Dr. Hernandez: "I understand, Emily. Can you tell me more about your symptoms?"
Emily: Describing her symptoms in detail "It's this dull ache in my lower abdomen, and it comes and goes. Sometimes it's sharp, and I've noticed some changes in my menstrual cycle too."
Dr. Hernandez: "Thank you for sharing that. Have you experienced any other symptoms, like abnormal bleeding or urinary issues?"
Emily: Nodding "Yes, occasionally. But nothing too severe."
Dr. Hernandez: "Based on what you've described, it's important to conduct a thorough assessment. I'd like to recommend some diagnostic tests, including a pelvic ultrasound and blood work, to help determine the underlying cause of your pelvic pain. Does that sound alright with you?"
Emily: Relieved "Yes, that sounds good. Thank you, Doctor."
Scenario 2: Rachel sat in the waiting room of her local gynecologist's office, nervously tapping her foot as she leafed through an outdated magazine.
Receptionist: "Rachel Summers? The doctor will see you now."
Rachel followed the nurse into the examination room, her heart pounding with anxiety.
Dr. Thompson: "Hello, Rachel. I'm Dr. Thompson. What seems to be the problem today?"
Rachel: Fidgeting "Hi, Doctor. I've been having this pelvic pain, and it's been bothering me for a while now."
Dr. Thompson: "Hmm. Can you describe the pain for me? How long have you been experiencing it?"
Rachel: Struggling to articulate her symptoms "It's kind of a dull ache, I guess. It comes and goes. Maybe for a few weeks now?"
Dr. Thompson: "Alright. Let's do a pelvic exam and some basic tests to start."
After a brief examination and some routine tests, Dr. Thompson concluded the appointment.
Dr. Thompson: "Well, Rachel, everything seems fine for now. Keep an eye on your symptoms, and if they persist, come back for a follow-up."
Rachel was about to ask Dr. Thompson another question, but the doctor stepped out of the room, shutting the door behind him. Rachel heard him shout at one of his nurses to be quicker when rooming his next patient.
Rachel left the office feeling uncertain and frustrated, her pelvic pain still unresolved.
In comparing Emily's experience with the online Ob/Gyn to Rachel's experience with the in-person Ob/Gyn, several advantages of seeking help online become evident. Emily was able to schedule her consultation quickly and conveniently, without the long wait times typical of in-person appointments. During her online consultation, Emily had ample time to fully discuss her symptoms with Dr. Hernandez, leading to a comprehensive assessment and appropriate diagnostic recommendations. In contrast, Rachel's in-person appointment felt rushed, and she left feeling uncertain about her next steps.
Additionally, the online consultation provided Emily with a sense of privacy and comfort, allowing her to discuss sensitive issues like pelvic pain from the comfort of her own home. Overall, Emily's experience highlights the benefits of seeking help from an online Ob/Gyn for pelvic pain, including convenience, accessibility, personalized care, and comprehensive assessment. Therefore, individuals experiencing pelvic pain should consider opting for an online doctor as the first step in seeking evaluation and treatment, as it can lead to better outcomes and a more satisfactory healthcare experience.

The absence of menstrual periods, known as amenorrhea, can be a cause for concern and may indicate underlying health issues. Consulting with an online Ob/Gyn doctor can offer valuable insights and assistance in addressing this condition.
But why opt for an online doctor over an in-person visit?
Consider the two following scenarios:
Scenario 1: Sarah, a 32-year-old woman, noticed that her menstrual periods had become irregular over the past few months, eventually leading to a complete absence of menstruation for the past three months. Concerned about her health, she decided to seek help from an online Ob/Gyn. During her virtual consultation, Sarah discussed her medical history, lifestyle factors, and the timeline of her menstrual irregularities in detail with the online doctor.
The online Ob/Gyn conducted a comprehensive assessment, asking Sarah about any associated symptoms, such as changes in weight, mood swings, or hot flashes. Based on her history, the doctor recommended diagnostic tests, including hormone assessments and thyroid function tests, to identify potential causes of her missed periods. Sarah was able to schedule these tests conveniently at a local laboratory and share the results with the online doctor.
Following the diagnostic evaluation, the online Ob/Gyn developed a personalized treatment plan tailored to Sarah's specific needs. This included lifestyle modifications, such as stress reduction techniques and dietary changes, as well as hormone therapy to regulate her menstrual cycle. Sarah appreciated the convenience of virtual follow-up appointments, where she could easily discuss her progress, ask questions, and adjust her treatment plan as needed without the hassle of scheduling in-person visits.
Scenario 2: Emily, also a 32-year-old woman, experienced similar menstrual irregularities and sought help from an in-person Ob/Gyn. After scheduling an appointment, she had to wait several weeks for an available slot, during which time her anxiety about her condition grew. When Emily finally met with the in-person doctor, she felt rushed during the appointment due to the doctor's busy schedule and limited time.
During the consultation, Emily provided her medical history and described her symptoms to the in-person Ob/Gyn. The doctor conducted a pelvic exam and recommended some basic blood tests but did not offer as detailed an assessment as Sarah experienced in her online consultation. Emily left the appointment feeling uncertain about her diagnosis and treatment plan.
Following the initial appointment, Emily had to wait several more weeks for the results of her tests and schedule a follow-up visit with the in-person Ob/Gyn. She found it challenging to coordinate her schedule with the doctor's availability and felt frustrated by the delays in receiving care.
In comparing Sarah's experience with the online Ob/Gyn to Emily's experience with the in-person Ob/Gyn, several key differences emerge. Sarah benefited from the convenience, timeliness, and accessibility of virtual consultations, allowing her to receive prompt evaluation and personalized treatment without the delays and scheduling difficulties associated with in-person visits.
The online Ob/Gyn provided a comprehensive assessment, recommended appropriate diagnostic tests, and developed a tailored treatment plan for Sarah's condition. With virtual follow-up appointments, Sarah could easily monitor her progress and adjust her treatment as needed, leading to better outcomes and a more positive overall experience.
Given the advantages of online consultations, individuals experiencing missed or absent periods should consider seeking help from an online Ob/Gyn first. By doing so, they can expedite the process of diagnosis and treatment, leading to better outcomes and improved reproductive health.

Heavy periods, medically known as menorrhagia, can significantly impact a woman's quality of life, causing discomfort, fatigue, and even anemia. But booking an appointment with a medical professional can be a lengthy process, as many Ob/Gyn physicians have full schedules.
For many people who are burdened with heavy periods, seeking help from a medical professional via telemed services can provide a fast, convenient, and effective solution– more importantly, it can even save you from the extra cost of seeing a doctor in person altogether.
Why Choose Online Help First?
Specifically, How Can an Online Ob/Gyn Help with Heavy Periods?
In sum, seeking help from an online Ob/Gyn doctor for heavy periods offers convenience, accessibility, and personalized care. By addressing your concerns virtually first, you can expedite the process of finding relief and managing your menstrual health effectively.

In the ever-evolving landscape of telehealth and digital health solutions, MIRA - Fertility Tracker has gained significant attention for its innovative approach to at-home health monitoring. However, it's crucial to shed light on a significant aspect that might be overlooked by users – MIRA doesn't employ doctors. This means that if you find yourself relying on MIRA for health and fertility insights without a reliable OBGYN familiar with MIRA, you might be left with data that are challenging to interpret accurately.
Biological data, especially when it comes to women's health, is complex and nuanced. Attempting to interpret such data in isolation can lead to misinterpretations and unnecessary concerns. Google might be a tempting source for self-diagnosis, but it's essential to recognize the limitations of trying to understand your health without the expertise of a qualified physician. Biological data cannot be properly interpreted so easily, and the guidance of a healthcare professional is invaluable in ensuring accurate understanding and appropriate actions.
In this context, My Virtual Physician stands out as a beacon of comprehensive women's health telemedicine. Unlike many other national telehealth companies that are one-trick ponies with limited scopes, My Virtual Physician offers full-scope gynecology services. Take NuRx, for example – its limitations in service offerings and the exclusion of insurance options make it clear that not all telehealth platforms are created equal.
What sets My Virtual Physician apart is the direct experience its gynecologists have in consulting with MIRA patients. This means that women using MIRA to track fertility can rest assured that the healthcare professionals at My Virtual Physician understand the intricacies of MIRA's data and can provide meaningful insights and guidance.
So, if you're a MIRA user facing the challenge of interpreting your data, consider booking a visit with My Virtual Physician. Our expertise, full-scope gynecology services, and direct experience with MIRA make us the go-to option for comprehensive and reliable healthcare in the era of digital health solutions. Your health is too important to be left to interpretation – trust the experts at My Virtual Physician to guide you through your health journey.
Telemedicine practices are on the rise, revolutionizing the way healthcare is delivered. However, a recent survey reveals that 55% of physicians find a misalignment between their patients’ expectations and what can be achieved through a virtual care model.
My Virtual Physician (MVP) stands out as an innovator, sharing the belief that virtual care can accomplish more for patients than ever before. While some providers offer a hybrid care model combining virtual and in-person visits, a hybrid model alone may not provide comprehensive care.
Let’s compare My Virtual Physician against Doctor on Demand, another popular telehealth provider, to see where MVP is breaking barriers in virtual healthcare.
Doctor on Demand is an established telemedicine provider offering virtual visits to treat specific conditions for patients. While they offer some primary care services, their scope of services is limited. Here’s a side-by-side comparison of treatment options:
| My Virtual Physician | Doctor on Demand | |
| Allergies | ✔️ | ✔️ |
| Earaches | ✔️ | ❌ |
| Cough, Cold, & Flu | ✔️ | ✔️ |
| Sinus Infection | ✔️ | ✔️ |
| Skin Rashes | ✔️ | ✔️ |
| Pediatric Care | ✔️ | ✔️ |
| Perinatal Care | ✔️ | ❌ |
| STD | ✔️ | ✔️ |
| Women’s Health | ✔️ | ✔️ |
| Irregular Periods | ✔️ | ❌ |
| Painful Periods | ✔️ | ❌ |
| Birth Control | ✔️ | ❌ |
| Infertility | ✔️ | ❌ |
| Menopause | ✔️ | ❌ |
| Acne | ✔️ | ✔️ |
| Mobile Testing | ✔️ | ❌ |
| Medical Marijuana | ✔️ | ❌ |
| Mental Health | ✔️ | ✔️ |
| Specialty Care | ✔️ | ❌ |
| Wound Care | ✔️ | ❌ |
| Chronic Condition Management | ✔️ | ❌ |
Doctor on Demand and My Virtual Physician are both complete care providers offering patients access to urgent care, primary care physicians, and pediatricians for online doctor appointments.
Another similarity between the two virtual providers is the availability of virtual and in-person visits. Doctor on Demand partners with certain facilities and helps patients find physical care providers.
My Virtual Physician, on the other hand, owns two clinics in Las Vegas with a care team employed on-site. They also provide virtual doctor visits to all 50 states offering a range from primary to specialty care physicians.
Doctor on Demand and My Virtual Physician appear to go toe-to-toe on paper until you start reading the fine print. That’s where MVP stands apart. My Virtual Physician is staffed with specialists, including:
And they are working to add even more specialist physicians for patients to have direct access to specialized care without a referral.
As far as pricing goes, Doctor on Demand comes with a bit of sticker shock. For a 15-minute virtual consultation for primary care, patients can expect to pay $79, while a 45-minute consultation with a Psychiatrist is nearly $300.
My Virtual Physician offers patients greater flexibility and a more straightforward pricing model. Visits are broken down into categories of acute, comprehensive, and specialty care. Depending on the nature of your visit, you’ll pay:
Reviews and ratings of telemedicine platforms provide valuable insights into patients’ experiences. Let’s address the elephant in the room between these two platforms. Doctor on Demand has a 1.5 rating on Trustpilot, indicating a significant number of negative experiences reported by users. Common complaints mention:
On the other hand, My Virtual Physician stands in stark contrast, boasting over 100 5-star reviews on Google. These positive ratings signify high satisfaction and appreciation from patients who have received care.
My Virtual Physician is no doubt the forerunner in revolutionizing healthcare through telemedicine, particularly for those in remote situations. They provide a total care approach for individuals with multiple chronic illnesses, using mobile teams of certified medical assistants (MA) and specialty physicians including OBGYNs, pediatricians, internists, and more.
This mobile team coordinates evaluations and consultations using an actual hybrid approach, where a medical assistant travels to the patient’s home with a tablet for video connections with doctors. The MA uses assistive technology to perform physical tasks such as:
Through the power of telemedicine, doctors can directly observe and supervise critical treatments, such as wound care, from the comfort of the patient’s own home. This convenient and inclusive approach breaks barriers ensuring individuals receive comprehensive care and specialized treatments regardless of their circumstances.
Doctor on Demand and My Virtual Physician both offer online telemedicine services, providing a range of treatment options and accessible healthcare services.
While Doctor on Demand caters to non-emergency medical conditions, mental health concerns, and general medical advice, My Virtual Physician takes it a step further by offering a more extensive and specialized approach to care.
The best thing about telemedicine is that patients can reach more providers now than ever possible before. This gives patients the power to choose from more than one provider for their healthcare needs. If you’re ready to check out what My Virtual Physician can do for you, our doctors are standing by to help.
Book Appointment Now Call For An Appointment
Women who have dedicated their lives to medicine may have an unsettling common denominator. Infertility in women is on the rise.
According to the American Medical Women’s Association, studies show that one in four female doctors struggle with infertility—that’s a whopping 25%.
Infertility is a growing problem. In the general population of the US, 19% of couples spend more than a year trying to get pregnant. For female doctors trying to start their families, the problem seems to be exacerbated.
If you’re a physician interested in learning more about your own fertility, we have resources for you. Learn more about fertility in our four-part blog series on testing for fertility indicators. For women working in higher-risk careers, it’s important to be proactive about fertility.

The exact reason that women in medicine face higher infertility rates is not clear. It’s likely a combination of factors. Below, we’ll outline a few likely culprits.
With each menstrual cycle that passes, the chance of getting pregnant decreases. A woman under the age of thirty has a 25-30% chance of pregnancy for each cycle. By a woman’s 40s, her chances of getting pregnant are reduced to 10% per cycle.
It’s well-known that age plays a role in women's fertility. It’s also common knowledge that it takes several years of education, training, and focus to become a doctor. Many women in medicine choose to delay starting a family during the years before becoming licensed to practice. The average age of a woman giving birth is 27, but for women physicians—it jumps up to 32 years old.
Medical school and residency often take up a dozen or so of a woman’s precious child-bearing years. By the time a woman reaches physician status, she’s likely already in her thirties and her ovarian reserve begins diminishing. We encourage women in medicine to see a fertility specialist. This is especially important for women over 30 who are trying for a baby.
It’s simple to see how it happens. Settling down to start a family often gets put on the back burner while your career launches, and before you know it, you’re nearing forty and still without a child. All this time, you may not have considered that your fertility may be compromised.
Related: Infertility: When is it Time to See a Doctor?
Who has time to settle down and find a mate when you’re busy trying to get trained on how to become a doctor? Busy schedules are another common reason that female doctors aren’t having babies as much as their non-physician counterparts. By the time you get back into the dating scene, your fertility has likely already peaked.
Other lifestyle factors that may play a role might include working in high-stress environments (although the relationship between stress and infertility is not well-understood), poor diet, lack of exercise, alcoholism, and more. The answer to the exact cause of the correlation between female physicians and infertility is still being studied.
Recognizing that there is a relationship between career choice and infertility is the first step to being proactive. Women in medicine must be informed that they are embarking on a career choice that could put them at a higher risk of infertility.
Even though women in medicine struggle more than others with infertility, there are proactive steps that can be taken to combat infertility in women.
Below are a few steps you can consider taking now:
If you’re currently struggling to conceive, our online OBGYNs can help with treating infertility.
If you’re a female physician who is concerned about this trend of women's infertility in the profession, My Virtual Physician is in your corner. We’re here to consult with you and provide answers. We can assist with regular fertility testing and our online OBGYNs serve patients in all 50 states.
If you’ve already received a concerning fertility test result, we’re available to consult with you on the best plan of action to move your fertility forward. Online appointments are available now; book your appointment today to meet with our board-certified OBGYNs.
Book Appointment Now Call For An Appointment
Need to see a specialist? Whether you’re looking for a Las Vegas OBGYN or a pediatrician for your child, getting established with a specialist physician can be an intimidating venture.
It used to be a lengthy, expensive, and convoluted process.
Luckily—things have changed. Today, there’s a new path available for patients. Now, you can see a healthcare specialist without the red tape.
More providers are paying attention to the patient experience, and a clear demand has surfaced: patients need easier access to specialists for healthcare. Healthcare specialist appointments must be easily accessible, swiftly scheduled, and transparently priced.
In this blog, we’ll define what specialists are and when you need to see them. And then, we’ll explore the processes required to see a healthcare specialist, both old and new—letting you in on the secret to seeing a Las Vegas Specialist in a snap.
When you call to schedule your appointment for your annual physical or a routine checkup, you’re likely booking with your primary care physician. These doctors can handle a wide range of common medical ailments seen in the general population.
A specialist, on the other hand, is a doctor who has expertise in a particular body system.
For example, an OBGYN specializes in the female reproductive system. Read more about the special care focus of an OBGYN below in the related blog at the link below.
Related: What’s an OBGYN: Get to Know Our Las Vegas Gynecology Team
An ENT doctor specializes in ailments of the ears, nose, and throat. A pediatrician specializes in the healthcare needs of children.
Here are some other specialists found in our healthcare system:
This is just a small selection of the many specialty fields out there in the world of healthcare.
There are many reasons to seek medical care from a healthcare specialist. Here are a few.
If you’re experiencing a chronic medical condition that your primary care doctor is unable to treat, it may be time to see a specialist. For example, if you’ve been asking your regular doctor to help clear up a skin condition, but it doesn’t seem to be improving—a dermatologist, who specializes in skin conditions, may be more qualified to help. Sometimes your doctor will refer you to a specialist; other times, you may need to seek out the specialist yourself.
Primary care physicians (PCPs) are trained to treat a broad scope of conditions that occur in the general population. If you know that you have a condition that is rare or that a specialist is more qualified to treat, then it may be appropriate to book directly with a specialist rather than a PCP. For example, if you have irregular menstrual cycles, an OBGYN or endocrinologist may be better able to pinpoint a care plan than a doctor with general training.
A third reason that patients desire to see a specialist is to find a doctor who is more familiar with treatment options that they have researched. If a primary care doctor is unfamiliar with a treatment that you want to try, seeing a specialist with experience using the treatment is a valid option.
So, now that you know when it’s time to see a specialist—let’s look at how to do it.
First, the long way.
Traditionally, the process of seeing a specialist involved making multiple appointments. Ultimately, your primary care physician was the gatekeeper who decided whether patients were permitted to schedule an appointment with a specialist.
Sometimes, you’d also need to have pre-approval from your insurance company before seeing a specialist. Insurance companies may deny coverage of specialist visits if the proper referral paperwork is not filed by your doctor’s office.
With the traditional method, you had to jump through hoops to see a specialist physician, including:
With the shortage of specialists in the Las Vegas area, seeing an OBGYN or other specialists in the area could take months.
Luckily, there’s a better way!
It’s hard to believe that anyone would follow the long process above to see a healthcare specialist when there’s such a simple shortcut. So, how can you see a specialist physician without jumping through hoops?
Schedule directly with your specialist.
My Virtual Physician wants patients to have access to specialists. That’s why we are here. Our patients have the option to visit with our Las Vegas specialists either online or inside our hybrid clinic located on Paradise Road in Las Vegas.
Our specialists include:
My Virtual physician offers transparent pricing and affordable visits for self-paying patients. Read more about grabbing affordable medications as a self-pay patient below.
Related: Guide to Self-Pay Prescriptions: Get the Best Price on Medications
If you’re located or visiting the Las Vegas area, walk-ins are welcome at our hybrid clinic. At this clinic, you can visit virtually with our specialists inside a private exam room right on the Vegas strip, making seeing a specialist on your own terms as easy as can be.
If you’re ready to book your appointment with one of our specialists, click below to self-schedule or walk into our hybrid clinic for an instant appointment. We look forward to serving you by providing a positive patient experience.
Book Appointment Now Call For An Appointment
You’ve been planning this vacation for months and now you’ve arrived—you finally made it to Vegas! Now, the fun begins…
You’re full of excitement and ready to experience the Vegas strip and have some fun! But there’s one detail that you probably didn’t plan out while you were booking tickets, packing your bags, and making your way to Nevada.
That detail is this—what to do if you need to see a doctor while you’re on vacation.
If you’re insured, seeing an out-of-state doctor may mean that you’ll face steep out-of-network charges that don’t count toward your regular deductible. If you’re uninsured, you might get stuck with hefty out-of-state medical bills.
If you’ve just arrived at your hotel in Las Vegas and realized you need to see a doctor ASAP, here’s what to do in order to see a doctor quickly and affordably so that you can turn your focus back to enjoying your vacation.
Before making any decisions, just pause for a moment. Focus on the reason that you need to see the doctor. If it’s because you forgot your medications at home, then write down the medications that you need refilled in Las Vegas to cover you during your vacation.
On the other hand, if you’re having indications of an illness that requires medication for you to feel better, write down your symptoms and how long you’ve had them. Some common illnesses that pop up during vacation include UTIs and bacterial infections.
If you feel a urinary tract infection (UTI) coming on or you are experiencing a sudden and extreme sore throat, write down your answers to the following questions:
In many cases, you’ll continue to feel miserable until you get antibiotics to fight the infection if it’s caused by bacteria. Tracking your symptoms as soon as you notice them can help you evaluate whether things are getting worse.
Related: What To Do If You Are Traveling With a UTI on Your Road Trip to Las Vegas
Take an account of the facts and assess the urgency of your situation before reacting. Once you’ve got your troubles documented, you can make an informed decision on whether or not you need to see a doctor.
The next step before taking action is to figure out the best type of doctor that can help you. A general practitioner can handle many common health concerns. But local doctors probably won’t have an opening for months and an urgent-care clinic staffed with general practitioners might cost you a small fortune in medical bills.
If your medical need requires a specialist, how can you find one in Vegas? Specifically, can you find an OBGYN in Las Vegas? OBGYNs specialize in the female reproductive system and cover anything from contraceptive prescriptions to menstrual problems and infertility. Read more about what conditions OBGYNs treat.
Once you’ve narrowed down whether it’s a general practitioner or a specialist that you need to see, you can start looking for a doctor or clinic. The two main places to look are in-person clinics in Las Vegas or online.
Telemedicine has provided greater access to healthcare and specifically, to specialists. Today, you can see a doctor in minutes rather than months. Searching for a provider online (who is licensed to practice in Nevada) can be one of the simplest solutions to finding a provider while traveling.
Online providers also tend to be more self-pay friendly. Since insurance companies don’t typically cover out-of-network providers, going online can be an affordable alternative. You’ll find a wide selection of specialists online who are taking new appointments.
Related: What to Expect During an online OBGYN Las Vegas Appointment
If you prefer a brick and mortar visit to the doctor without breaking the bank, My Virtual Physician has created a hybrid clinic to meet that need. Located on Paradise Road in Las Vegas, this clinic offers televisits for walk-ins and same-day appointments. Appointments are available for a flat, affordable price. Get back to the fun after stopping by the hybrid clinic on Paradise Road.
Our hybrid clinic is staffed virtually with a variety of physicians and specialists (including pediatricians and OBGYNs) to help you get feeling better faster.
If you’ve been prescribed medication during your hybrid or telemedicine visit, picking it up is also a simple process. You’ll need to find a Las Vegas pharmacy that is nearby so that you can get your prescription right away. There are several pharmacies within walking distance of our hybrid clinic where your doctor can send your prescription to be filled.
For help finding the most affordable local pharmacy, check out our guide to self-pay prescriptions below.
Related: Guide to Self-Pay Prescriptions: Get the Best Price on Medications
My Virtual Physician is proud to provide greater access to doctors and specialists, particularly in the Las Vegas area with our hybrid clinic on Paradise Road. Our board-certified Las Vegas team of OBGYNs, pediatricians, and other specialists are here to help if you find yourself needing to see a doctor urgently while on vacation in Las Vegas or elsewhere.
Walk into our hybrid clinic today or schedule your online appointment now by clicking below.
Book Appointment Now Call For An Appointment
Need to get in to see your OBGYN?
There are a lot of reasons to see your OBGYN, including getting contraceptive refills, screenings, and care for menstrual concerns, infertility, menopause, sexual health, urinary problems, and pregnancy.
For most women, scheduling a gyno appointment comes with a feeling of dread. But this Las Vegas OBGYN clinic is making life easier than ever for women in the big city.
Find out how you can see your gynecologist in a matter of minutes, right here in Vegas.
There’s a lot that can get out of whack with a woman’s body if left untreated. Here’s a quick list of signs that will grab your attention until treated. Do not delay your visit to the gynecologist if you have any of the following issues:
Related: Our Las Vegas OBGYNs Cure Your Bacterial Vaginosis Fast
These are all signs that you need to see your OBGYN urgently. But how can you make that happen?
Here’s the secret to getting your OBGYN appointment quicker: forget the traditional appointment model.
In the past, seeing your gynecologist was something that had to be planned well in advance. First, you’d have to get established with a brick-and-mortar healthcare facility before you were allowed to see a specialist at all.
Next, you’d have to call and schedule an appointment. It’s not unusual for specialists like OBGYNS to be booked out for months—especially in Las Vegas. If you’re lucky, your gynecologist might try to squeeze you in between patients if you have an urgent need. But you’ll probably be waiting around for hours to be seen.
So, what’s a girl to do? There’s got to be a quicker way for getting in to see a Las Vegas OBGYN. Luckily, there is.
Telemedicine is paving the way for quicker access to your doctor, bypassing the dreadful waiting that accompanies traditional appointments.
Thanks to the increasing availability of telemedicine, you can now see your doctor in a less traditional way: online. And it’s not just your primary care physicians that have moved their practices into the digital space. Specialists, including obstetricians and gynecologists, are making appointments accessible to patients online.
There’s no denying that telemedicine is increasing access to care exponentially. Now, you can see your Las Vegas OBGYN on your terms and from the comfort of your own home. In the digital realm, doctors are able to reach more patients, spread the demand for care over a wider supply of physicians, and complete appointments from start to finish more efficiently. It’s a win-win situation.
Related: Telemedicine Improves Access to Prenatal Care, But Can We Improve Access to Telemedicine?
But beaming up your doctor on your smartphone or computer doesn’t work for everyone. And for those patients who prefer to come into a physical facility, My Virtual Physician is providing an alternative called a hybrid clinic.
My Virtual Physician has opened a new type of healthcare facility. Their hybrid clinic, located on Paradise Road in Las Vegas, provides patients a way to virtually meet with an OBGYN, pediatric, or primary care physician on a walk-in basis.
Inside the clinic, you’ll find a certified medical assistant who will walk you through the steps to visit virtually with our doctors in a private room. Our assistant can also measure your vitals during your visit. Ultrasounds and other specialist appointments can also be scheduled ahead of time at the hybrid clinic.
My Virtual Physician is making Las Vegas OBGYN care more accessible to patients in the city who prefer a healthy mix between traditional visits and speed. Visit us today for a transparently affordable visit with our specialists.
Holiday traditions encourage families to get together to celebrate with distant relatives—including aunts, uncles, grandparents, and in-laws. This is an opportunity to catch up with one another and find out how everyone in your family has been doing since you were last together.
Family get-togethers are also a suitable occasion to recognize when something isn’t quite right. This season provides a short window of opportunity for intervention when someone is crying out for help from elder abuse.
In this article, we aim to spread awareness about elder abuse during this holiday season by covering:
Elder abuse is when a trusted caregiver knowingly or negligently takes advantage of an elder—it can include physical or sexual abuse—or take another form, such as:
The elderly tend to be more vulnerable to abuse than other adults. That’s because there is a gradual decline in physical strength and mental acuity as we age. Many of our elders also depend on caregivers to help with day-to-day functioning.
According to the American College of Obstetricians and Gynecologists, as many as one in ten adults over the age of 60 may become a victim of elder abuse. And only around 1 in 23 cases of elder abuse are reported to authorities. With such a high incidence, it’s critical to know what to look for to spot elder abuse.
Doctors often screen for signs of elder abuse during regular visits, and the ACOG recommends that OBGYNs screen all patients over the age of 60 for signs of abuse.
But doctors are not the only ones who can recognize the signs of abuse. When you meet with your loved ones this holiday season, look deeper at any red flags that grab your attention.
For example, if your grandpa shows up to Christmas dinner with teeth missing from his dentures and unkempt hair, you might begin to look for other signs that he is not receiving proper care. If your aunt, who takes care of grandpa, has a shiny new car out of the blue and a bad attitude toward grandpa—that’s worth investigating further.
Here are some other signs to look out for:
If you notice any of these signs, it’s worth investigating whether your family member has become a victim of elder abuse. Talking to your loved one directly about the red flags may not be enough to get them the help they need—so what can you do to get real help if you suspect elder abuse?
Our elders deserve protection. If you suspect elder abuse, the best course of action is to report it to authorities, who are trained to investigate this type of situation. You can report suspected abuse to a number of agencies, including:
The National Center on Elder Abuse website has state-specific resources for you to contact the right professionals in order to get help in your region.
If you’re not sure whether your loved one is suffering from abuse, you can encourage your elder to see his or her doctor, who will do an elder abuse screening. Physicians are mandated reporters, which means that they must report suspected abuse to authorities.
Sadly, elder abuse is not an uncommon occurrence. But the good news is that everyone has the ability to do their part to help stop the abuse. Simply reporting any suspicions to the proper authorities may be enough to put an end to elder abuse.
My Virtual Physician prioritizes protecting vulnerable populations and can help with the reporting process. Contact us today if you or a loved one needs help.

Imagine a world where you can’t get in to see your doctor for months or even years. Whether you simply need a prescription refill or help diagnosing and managing a chronic medical condition like diabetes, both can produce scary, or even life-threatening, scenarios.
Now, consider that the United States isn’t that far from this reality. In a 2021 report, the Association of American Medical Colleges (AAMC) predicted that a physician shortage is coming to the US. By 2034, the country will fall short of meeting the appropriate physician-to-patient ratios.
In fact, the AAMC believes that the US will fall between 40,000 to 124,000 doctors short in the next decade or so.
It makes sense that densely-populated areas require more doctors in order to meet healthcare needs. That’s where the physician-to-patient ratio comes in. If you can measure this ratio, it tells you whether you have enough doctors to meet a geographical area’s healthcare needs.
Most states within the USA fall below the ideal physician-to-patient ratio. An ideal number is around 270 physicians per 100,000 people. This equates to about 370 patients per doctor. Many states hover around a rate closer to 200:100,000.
The governmental agency known as the Health Resources & Services Administration (HRSA) works to increase healthcare access to vulnerable populations (geographically isolated, economically or medically vulnerable). Reports are available on their website. These reports show where vulnerable populations are located and where physicians are needed the most.
Nevada has been experiencing a physician shortage for some time. Currently, the state’s ratio remains around 200:100,000. Read more here about the OB/GYN Physician Shortage in Las Vegas.
HRSA reports displaying Health Professional Shortage Areas (HPSA) show regions where there is a shortage of providers. Nevada shows 75 areas with a primary care physician shortage, plus numerous dental and mental health areas where there is a shortage of specialists to serve these populations.
A search on medically underserved areas from HRSA shows 25 regions within the state have underserved areas and populations. Specifically, these areas in Las Vegas are underserved:
It is My Virtual Physician’s mission to provide access to healthcare for men, women, and children. That’s why we offer online telemedicine visits for patients in any US state. This helps break down geographical barriers in order to increase the real physician-to-patient ratio. On top of that, we have taken it a step further with our hybrid clinic located in Las Vegas.
Read about our hybrid clinic’s opening here: My Virtual Physician Celebrates Las Vegas Hybrid Clinic Opening.
This clinic helps to serve populations who may not have access to the digital requirements of telemedicine. We provide a private room that our patients can use to meet virtually with our doctors inside the clinic located at 2217 Paradise Road in Las Vegas.
Additionally, the clinic provides immediate access for all populations. Walk-ins are welcome during business hours. Find out more here. Our doctors can provide primary care needs as well as specialty visits. In addition to our primary care doctors, we also have board-certified OBGYNs and Pediatricians ready to meet with patients.

My Virtual Physician has an exciting announcement to celebrate: our hybrid clinic on Paradise Road is now open in Las Vegas!
My Virtual Physician’s mission is to provide safe, secure, and convenient access to healthcare for men, women, and children. In other words, we use telemedicine to fill the healthcare access gap that’s left by the reality that many doctors don’t offer same-day services. Patients who need to see a doctor now have the ability to meet virtually with our team of physicians with same-day appointments.
Our online telemedicine services launched during the pandemic, have grown exponentially, and continue strong today—providing quality healthcare access nationwide, online. We credit our growing team of doctors for our success.
But My Virtual Physician aims higher than simply providing online access to those who have the right equipment for a virtual visit (such as a smartphone or computer equipped with a camera and mic).
Other limitations exist with providing this type of healthcare solely online, including not having a private or safe place to interact virtually and the lack of medical equipment for taking vitals and collecting labs for diagnostics.
To overcome this challenge, My Virtual Physician opened its first one-of-a-kind hybrid clinic in Las Vegas. We’re excited to announce that, despite some major obstacles, we have successfully launched our first physical walk-in location.
Related: Hybrid Medical Clinics: Expanding OBGYN Access in Las Vegas
My Virtual Physician’s hybrid medical clinic is now open at 2217 Paradise Road in Las Vegas. Walk-ins are welcome. Find out our current hours or book an appointment (if preferred) here.
We are pleased to welcome men, women, and children into the physical clinic for a virtual visit in our private patient room, where our videoconferencing equipment is already set up and ready to go. We provide women’s health, pediatric, and primary care services in our hybrid clinic.
My Virtual Physician is proud to have opened the first clinic in Vegas that offers immediate access to online healthcare for those who may not have access to the equipment or private space. We welcome all to come visit us. Find us on Paradise Road! Get Directions Here.
Related: Now Available: Walk-in STD Testing in Las Vegas at Hybrid Clinic
 Inside Our Las Vegas Hybrid Clinic
Inside Our Las Vegas Hybrid ClinicTake a peek inside our clinic, where our certified medical assistant (CMA) will greet you! We have a comfortable waiting room for busier times. We also have a private room for patient use where our CMA will take your vitals, give you the tools to collect samples if needed for labs, and then you can meet virtually with our doctors with our private and secure videoconferencing setup.
At times, we do staff the clinic with a nurse manager and other medical professionals who can provide additional services such as wound care, vaccinations, ultrasounds, and more. If you’re interested in these services, please call ahead to (888) 224-0804 so that we can make sure the appropriate staff is present for your visit.
My Virtual Physician offers affordable and immediate access to patients at our new hybrid clinic in Las Vegas. Click to find out more about which services we offer. Welcome to our clinic!